277 results
193 Beyond Independence: The Empowering Potential of an Assistive Technology Web App to Enrich the Lives of Older Latinos with Functional Disabilities
- Part of
- Elsa M. Orellano-Colon, Wency Bonilla-Díaz, Radamés Revilla-Orellano, Jesús Mejías-Castro, Josí Torres-Irizarry, Nixmarie Figueroa-Alvira, Angelis M Fernández-Torres, Bernice Ortiz-Vélez, Gabriela A. Torres-Ferrer, Nina L. Rivera-Rivera
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue s1 / April 2024
- Published online by Cambridge University Press:
- 03 April 2024, p. 59
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/GOALS: The use of assistive technology (AT) devices is known to improve older adults’ independence in daily activities. However, little is known about the impact of using an AT web app in older Latinos’ life. This study aims to evaluate the value and usefulness of the My Assistive Technology Guide web app among older Latinos with physical function disabilities. METHODS/STUDY POPULATION: We employed a convergent parallel mixed-method design with 12 community-living older Latinos from Puerto Rico. Researchers provided training in the use of My Assistive Technology Guide, a Spanish evidence-based web app with detailed information on 97 AT devices and videos of older people using them. Participants were encouraged to use it for 30 days. Afterward, we collected quantitative data using the subjective quality domain of the User Mobile Application Rating Scale (uMARS), followed by qualitative data through individual interviews. Quantitative data were analyzed with descriptive statistics and qualitative data with thematic content analysis. RESULTS/ANTICIPATED RESULTS: My Assistive Technology Guide web app received high ratings in the uMARS subjective quality domain (mean 4.5 [SD 0.5] out of 5), indicating that participants highly valued the usefulness of the web app. Qualitative data fell into four main categories: functional health, meaningful participation, autonomy, and personal growth. DISCUSSION/SIGNIFICANCE: The findings suggest that the AT knowledge provided by the My Assistive Technology Guide web app has the potential to enhance the quality of life of older Latinos in the face of the challenges posed by physical function disabilities as people age.
22 Cordoba Naming Test Performance and Acculturation in a Geriatric Population
- Isabel C.D. Muñoz, Krissy E. Smith, Santiago I. Espinoza, Diana M. R. Maqueda, Adriana C. Cuello, Ana Paula Pena, Carolina Garza, Raymundo Cervantes, Jill Razani, Tara L. Victor, David J. Hardy, Alberto L. Fernandez, Natalia Lozano Acosta, Daniel W. Lopez-Hernandez
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 335-336
-
- Article
-
- You have access Access
- Export citation
-
Objective:
A commonly used confrontation naming task used in the United States is The Boston Naming Test (BNT). Performance differences has been found in Caucasian and ethnic minorities on the BNT. The Cordoba Naming Test (CNT) is a 30-item confrontation naming task developed in Argentina. Past research has shown acculturation levels can influence cognitive performance. Furthermore, one study evaluated geriatric gender differences on CNT performance in Spanish. Researchers reported that older male participants outperformed female participants on the CNT. To our knowledge, researchers have not evaluated ethnic differences on the CNT using a geriatric sample. The purpose of the present study was to examined CNT performance and acculturation in a Latinx and Caucasian geriatric sample. It was predicted the Caucasian group would outperform the Latinx group on the CNT. Moreover, the Caucasian group would report higher acculturation levels on the Abbreviated Multidimensional Acculturation Scale (AMAS) compared to the Latinx group.
Participants and Methods:The sample consisted of 9 Latinx and 11 Caucasian participants with a mean age of 66.80 (SD =6.10), with an average of 14.30 (SD = 2.00) years of education. All participants were neurologically and psychologically healthy and completed the CNT and the AMAS in English. Acculturation was measured via the AMAS English subscales (i.e., English Language, United States. Identity, United States, Competency). A series of ANCOVAs, controlling for years of education completed and gender, was used to evaluate CNT performance and acculturation.
Results:The ethnic groups were not well demographically matched (i.e., years of education and gender).We found that the Caucasian group outperformed the Latinx group on CNT performance p = .012, ηp 2 = .34. Furthermore, the Caucasian group reported higher acculturation levels (i.e., English Language, United States, Identity, United States, Competency) compared to the Latinx group p’s < .05, ηps2 = .42-.64.
Conclusions:To our knowledge, this is the first study to evaluate CNT performance between ethnic groups with a geriatric sample. As expected the Caucasian group outperformed the Latinx group on the CNT. Also, as expected the Caucasian group reported higher English acculturation levels compared to the Latinx group. Our findings are consistent with past studies showing ethnic differences on confrontational naming performance (i.e., The Boston Naming Test), favoring Caucasians. A possible explanation for group differences could have been linguistic factors (e.g., speaking multiple languages) in our Latinx group. Therefore, since our Latinx group reported lower levels of English Language, United States identity, and United States competency the Latinx group assimilation towards United States culture might of influence their CNT performance. Future studies with different ethnic groups (e.g., African-Americans) and a larger sample size should examine if ethnic differences continue to cross-validate in a geriatric sample.
30 Analyzing Spanish Speakers Cordoba Naming Test Performance
- Raymundo Cervantes, Isabel D.C. Munoz, Estefania J. Aguirre, Natalia Lozano Acosta, Mariam Gomez, Adriana C. Cuello, Krissy E. Smith, Diana I. Palacios Mata, Krithika Sivaramakrishnan, Yvette De Jesus, Santiago I. Espinoza, Diana M. R. Maqueda, David J. Hardy, Tara L. Victor, Alberto L. Fernandez, Daniel W. Lopez-Hernandez
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 443-444
-
- Article
-
- You have access Access
- Export citation
-
Objective:
A 30-item confrontation naming test was developed in Argentina for Spanish speakers, The Cordoba Naming Test (CNT). The Boston Naming Test is an established confrontation naming task in the United States. Researchers have used the Boston Naming Test to identify individuals with different clinical pathologies (e.g., Alzheimer’s disease). The current literature on how Spanish speakers across various countries perform on confrontational naming tasks is limited. To our knowledge, one study investigated CNT performance across three Spanish-speaking countries (i.e., Argentina, Mexico, and Guatemala). Investigators found that the Guatemalan group underperformed on the CNT compared to the Argentine and Mexican groups. The purpose of this study was to extend the current literature and investigate CNT performance across five Spanish-speaking countries (i.e., Argentina, Mexico, Guatemala, Colombia, United States). We predicted that the Argentine group would outperform the other Spanish-speaking countries.
Participants and Methods:The present study sample consisted of 502 neurologically and psychologically healthy participants with a mean age of 29.06 (SD = 13.41) with 14.75 years of education completed (SD = 3.01). Participants were divided into five different groups based on their country of birth and current country residency (i.e., United States, Mexico, Guatemala, Argentina, & Colombia). All participants consented to voluntary participation and completed the CNT and a comprehensive background questionnaire in Spanish. The CNT consisted of 30 black and white line drawings, ranging from easy to hard in difficulty. An ANCOVA, controlling for gender, education, and age, was used to evaluate CNT performance between the five Spanish-speaking country groups. Meanwhile, a Bonferroni post-hoc test was utilized to evaluate the significant differences between Spanish-speaking groups. We used a threshold of p < .05 for statistical significance.
Results:Results revealed significant group differences between the five Spanish speaking groups on the CNT, p = .000, np2 = .48. Bonferroni post-hoc test revealed that the United States group significantly underperformed on the CNT compared to all the Spanish-speaking groups. Next, we found the Guatemalan group underperformed on the CNT compared to the Argentinian, Mexican, and Colombian groups. Additionally, we found the Argentinian group outperformed the Mexican, Guatemalan, and United States groups on the CNT. No significant differences were found between the Argentinian group and Colombian group or the Mexican group and Colombian group on the CNT.
Conclusions:As predicted, the Argentinian group outperformed all the Spanish-speaking groups on the CNT except the Colombian group. Additionally, we found that the United States group underperformed on the CNT compared to all the Spanish-speaking groups. A possible explanation is that Spanish is not the official language in the United States compared to the rest of the Spanish-speaking groups. Meanwhile, a possible reason why the Argentinian and Colombian groups demonstrated better CNT performances might have been that it was less culturally sensitive than the United States, Mexican, and Guatemalan groups. Further analysis is needed with bigger sample sizes across other Spanish-speaking countries (e.g., Costa Rica, Chile) to evaluate what variables, if any, are influencing CNT performance.
Ten New Insights in Climate Science 2023/2024
- Mercedes Bustamante, Joyashree Roy, Daniel Ospina, Ploy Achakulwisut, Anubha Aggarwal, Ana Bastos, Wendy Broadgate, Josep G. Canadell, Edward R. Carr, Deliang Chen, Helen A. Cleugh, Kristie L. Ebi, Clea Edwards, Carol Farbotko, Marcos Fernández-Martínez, Thomas L. Frölicher, Sabine Fuss, Oliver Geden, Nicolas Gruber, Luke J. Harrington, Judith Hauck, Zeke Hausfather, Sophie Hebden, Aniek Hebinck, Saleemul Huq, Matthias Huss, M. Laurice P. Jamero, Sirkku Juhola, Nilushi Kumarasinghe, Shuaib Lwasa, Bishawjit Mallick, Maria Martin, Steven McGreevy, Paula Mirazo, Aditi Mukherji, Greg Muttitt, Gregory F. Nemet, David Obura, Chukwumerije Okereke, Tom Oliver, Ben Orlove, Nadia S. Ouedraogo, Prabir K. Patra, Mark Pelling, Laura M. Pereira, Åsa Persson, Julia Pongratz, Anjal Prakash, Anja Rammig, Colin Raymond, Aaron Redman, Cristobal Reveco, Johan Rockström, Regina Rodrigues, David R. Rounce, E. Lisa F. Schipper, Peter Schlosser, Odirilwe Selomane, Gregor Semieniuk, Yunne-Jai Shin, Tasneem A. Siddiqui, Vartika Singh, Giles B. Sioen, Youba Sokona, Detlef Stammer, Norman J. Steinert, Sunhee Suk, Rowan Sutton, Lisa Thalheimer, Vikki Thompson, Gregory Trencher, Kees van der Geest, Saskia E. Werners, Thea Wübbelmann, Nico Wunderling, Jiabo Yin, Kirsten Zickfeld, Jakob Zscheischler
-
- Journal:
- Global Sustainability / Accepted manuscript
- Published online by Cambridge University Press:
- 01 December 2023, pp. 1-58
-
- Article
-
- You have access Access
- Open access
- Export citation
Night-time/daytime Protein S100B serum levels in paranoid schizophrenic patients
- E. Diaz-Mesa, A. Morera-Fumero, L. Torres-Tejera, A. Crisostomo-Siverio, P. Abreu-Gonzalez, R. Zuñiga-Costa, S. Yelmo-Cruz, R. Cejas-Mendez, C. Rodriguez-Jimenez, L. Fernandez-Lopez, M. Henry-Benitez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S445-S446
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
S100B is a calcium-binding astrocyte-specific cytokine, that is considered a biomarker of neurodegeneration; which may be involved in the imbalance of the inflammatory response observed in several brain disorders, including major depression and schizophrenia. Two meta-analyses have reported higher serum levels of S100B in patients with schizophrenia respect to healthy controls.
Different studies have described circadian and seasonal variations of biological variables, such as melatonin or cortisol. It has been reported that there is not circadian rhythm of S100B blood levels in healthy subjects. However, it is not known whether there are circadian oscillations in S100B blood concentrations in patients with schizophrenia.
ObjectivesThe aim of this study is to describe S100B serum levels in patients with schizophrenia and to analyse whether they follow a circadian rhythm.
MethodsOur sample consists in 47 patients in acute phase and stabilized status. Blood samples were collected at 12:00 and 00:00 hours by venipuncture. Serum levels of Protein S100B were measured three times: at admission, discharge and three months after discharge. Protein S100B was measured by means of ELISA (Enzyme-linked immunosorbent assay) techniques.
Results12:00 24:00 P ADMISSION 132,95±199,27 85,85±121,44 0,004 DISCHARGE 73,65±71,744 75,80±123,628 0,070 CONTROL 43,49±34,60 40,14±23,08 0,47 P global P Admission Vs. Discharge P Admission Vs. Control P Discharge Vs. Control 0,97 There is a significance difference between 12:00 and 24:00 at admission for the Protein S100B.However, these difference did not occur at discharge and at three months after discharge.It can be interpreted as there is a circadian rhythm of Protein S100B when the patient has got a psychotic outbreak and disappears at discharge and when is psychopathologically stable.
ConclusionsWith respect to our results we can hypothesize that schizophrenic patients in acute relapse present circadian S100B rhythm that is not present when the patients are clinically stable.Furthermore, the decrease of serum protein S100B levels at discharge is indicative of a reduction of the cerebral inflammation, thus it can be a biomarker of cerebral inflammation and this reduction can be the effect of the treatment. Finally, its circadianity could be a guide of this process and clinical improvement.
Disclosure of InterestNone Declared
PSYCHIATRIC COMORBIDITY IN A SAMPLE OF PATIENTS WITH COGNITIVE-BEHAVIORAL MINORITY DISEASE
- R. De la Mata, C. Manso-Bazús, S. Pujol, L. Torrent, L. Urraca, D. Vázquez-Tarrio, M. Esteve, E. Fernández, M. Pàmias
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S743
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
About the term cognitive-behavioral minority disease or rare disease are a group of diseases that affect between 6-8% of the populatio. It is estimated that there are more than 7000 in the world, the majority with a genetic basis and affect various organs and systems, they also present psychiactric comorbidities and cause a physical or mental disability. Given its definition, it is difficult to see a large number of these patients in our usual clinical activity, so their management can be complicated.
ObjectivesTo evaluate the prevalence of psychiatric comorbidity and the prevalence of psyhcopharmacological treatment in children and adolescents whe present a minority disease.
MethodsThis is a descriptive, controlled, retrospective cross-sectional study of a sample obtained by non-probabilistic sampling, which is representative of the study population.
The statistical analysis was made using the statistical program SPSS V22 (2013).
ResultsWith a sample of 114 patients, of which 26,6% presented fragile X syndrome, secondly 25,3% presented Prader-Willi Syndrome and 48,1% other chromosomal abnormalities.
By subgroups (male:female): in Prader-Willi syndrome 6:14 (30%:70%), in Fragile X syndrome 12:9 (57,14%: 42,86%) and in other diseases 25:13 (75,69%: 34,21%).
ConclusionsThe creation of clinical expert units makes the possibility to increase knowledge of diseases whose prevalence in the population, thanks to technological advances, is increasing and where scientific knowledge is still limited.
These units are also important, in order to be able to offer personalized intensive treatments in order to reduce polypharmacy. There is not a great difference between the minority diagnosis and polypharmacy, although there is less polypharmacy than expected, which may be the result of the success of the most intensive and personal psychotherapeutic intervention in the unit.
Disclosure of InterestNone Declared
Do attention-deficit/hyperactivity symptoms influence treatment outcome in gambling disorder?
- C. Vintró-Alcaraz, G. Mestre-Bach, R. Granero, M. Gómez-Peña, L. Moragas, F. Fernández-Aranda, M. N. Potenza, S. Jiménez-Murcia
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S58-S59
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Numerous studies point to the comorbidity between gambling disorder (GD) and attention deficit hyperactivity disorder (ADHD). However, there is a lack of research exploring how ADHD symptoms might influence psychological treatment outcomes for GD.
ObjectivesTherefore, we aimed to explore differences between patients with GD with and without ADHD symptoms regarding psychopathology, personality, sociodemographic and especially treatment outcome measures.
MethodsThis longitudinal study included n=170 patients with GD receiving 16 sessions of cognitive behavioral therapy (CBT) in a specialized unit of a public hospital. Multiple self-reported instruments were used to assess GD severity, personality, ADHD and other symptoms and sociodemographic measures prior to treatment.
ResultsA clinical profile characterized by greater GD severity, higher psychopathology and impulsivity, and less adaptive personality features was observed in patients with self-reported ADHD symptoms compared to those without. No significant differences in treatment response (measured by dropout and relapse rates) were reported between the two groups. However, patients with ADHD symptoms described more severe relapses (more money gambled) and GD patients who relapsed scored higher on measures of ADHD, particularly inattention.
ConclusionsIndividuals with GD and ADHD may experience more severe relapses following treatment, suggesting a need for more vigilant follow-up and interventions for patients with this comorbidity.
Disclosure of InterestC. Vintró-Alcaraz: None Declared, G. Mestre-Bach: None Declared, R. Granero: None Declared, M. Gómez-Peña: None Declared, L. Moragas: None Declared, F. Fernández-Aranda Consultant of: Novo Nordisk and editorial honoraria as EIC from Wiley, M. Potenza Consultant of: Opiant Pharmaceuticals, Idorsia Pharmaceuticals, AXA, Game Day Data, Baria-Tek and the Addiction Policy Forum; has been involved in a patent application with Yale University and Novartis; has received research support (to Yale) from Mohegan Sun Casino and Connecticut Council on Problem Gambling; and has consulted for and/or advised gambling and legal entities on issues related to impulse-control/addictive disorders, S. Jiménez-Murcia: None Declared
DOCTOR, I’M PREGNANT. Psychopharmacological treatment of depression in pregnant women. A clinical case of a pregnant woman and major depressive disorder
- M. Queipo De Llano De La Viuda, G. Guerra Valera, C. Vallecillo Adame, C. De Andrés Lobo, T. Jiménez Aparicio, M. Fernández Lozano, I. D. L. M. Santos Carrasco, N. De Uribe Viloria
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1011
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Depression during pregnancy can appear with a prevalence of up to 11% of pregnant women. Psychotherapeutic treatment in these cases is considered the first option, but treatment with antidepressants is sometimes required in these cases.
ObjectivesTo present a clinical case of a pregnant patient diagnosed with depression.
MethodsLiterature review of the psychopharmacological treatment of depression during pregnancy and possible complications.
ResultsA 25y Year old woman, 22 weeks pregnant, who lives with her partner. She has no background in mental health. Paternal aunt diagnosed with type I Bipolar Disorder. She goes to the Mental Health Center for evaluation, due to anxiety and depressive symptoms of 4 weeks of evolution, she refers sadness and apathy, continuous crying, somatic anxiety and obsessive ruminations in relation to childbirth and inability to care for your child. Suicidal ideation as a resolution of her discomfort. She presents with global insomnia and a significant loss of appetite, with a weight loss of 3 kg. Treatment with sertraline 50 mg/day was started, with good tolerance and clinical response
ConclusionsThe psychopharmacological treatment of antenatal depression is a challenge for the psychiatric professional. In all cases, an adequate balance must be made between the risks and complications for the fetus and the psychopathological stability of the pregnant woman. Among the main risks of untreated depression are: preterm delivery and low birth weight, an increased risk of suicide and alterations in the development during the baby’s infancy. The most used antidepressants are the SSRIs, with sertraline being a good option. Paroxetine has been associated with cardiac defects in the newborn. There are studies with tricyclics and duals but no specific teratogenic pattern has been seen. They are associated with an increased risk of spontaneous abortion. Exposure during the third trimester may be associated with obstetric complications.
Disclosure of InterestNone Declared
A cross-sectional descriptive study to assess the impact of the “open door” policy on patient satisfaction
- M. Campillo, J. Marti, L. Rius, S. Garcia Fernandez, M. Olivero, G. Sanchez Tomico, G. Brusco-Passalaqua, E. Pechuan, T. Vates, R. Sanchez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S910
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Since the beginning of the modern psychiatry the acute units have established a “locked door” policy. Some studies show that this condition may increase patient’s discomfort and affect the perception of health quality of care (Boyer L, 2009, Eur Psychiatry Dec;24(8):540-9). Lately, several European countries such as Germany, Switzerland and Spain are starting to implement the “open-door” policy but its impact on patient’s satisfaction is still unknown (Hochstrasser, L, Frontiers in Psychiatry, 9(57). https://doi.org/10.3389/fpsyt.2018.00057) .
ObjectivesTo help characterize the advantages of the “open-door” policy implemented in an acute inpatient psychiatric unit in order to assess the patient’s view of it.
MethodsThis is a descriptive observational study carried out at an inpatient psychiatric unit. Data were collected after the implementation of the open door policy on June 2019, assessing the patient satisfaction of 31 subjects who completed the SATISPSY-22 scale at the time of discharge. Results are described using the average and its standard deviation.
ResultsResults show scores in all items above 50 points, being the care team and the quality of care the most valued ones with 82 and 79 points respectively. The overall score is above 65 points (Fig. 1).
Image:
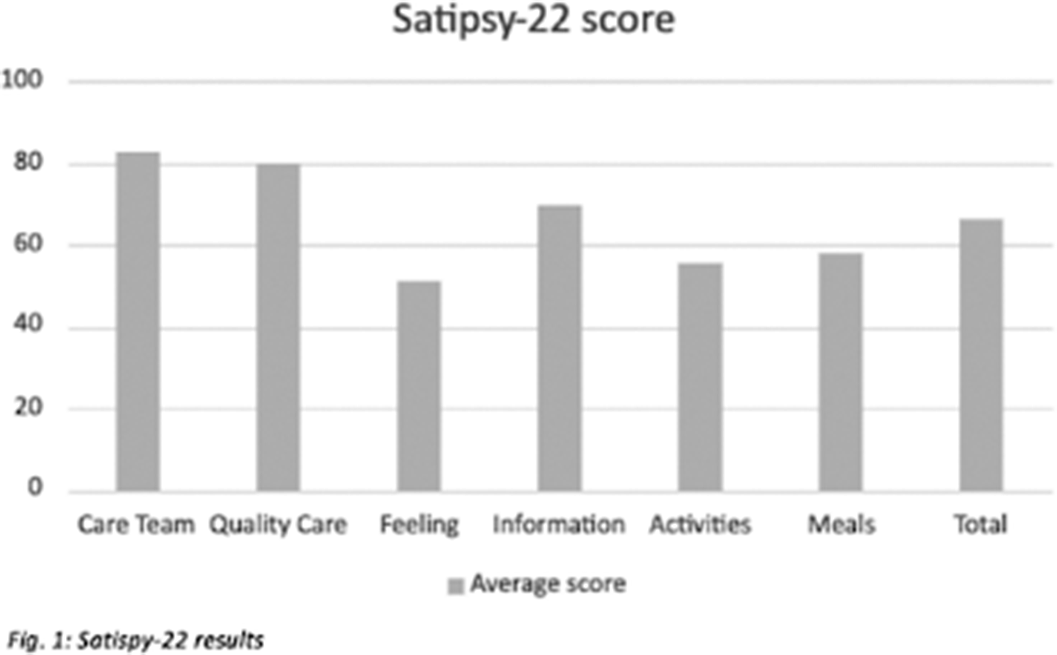 Conclusions
ConclusionsIn line with previous studies, our data suggests that the main impact of the “open-door” policy implementation is on patients’ perception of the care, being Quality of care and satisfaction with the Staff the items with highest scores. This could be explained by patients trusting more in the Care team, which would help enhance the therapeutic relationship improving therapeutic adherence, treatment adequacy and the outcome. Nevertheless, the Feeling related to hospitalisation was found to be the item with the lowest score. This could mean strategies should focus on improving patient’s insight regarding their clinical state and their need to be admitted. Our study supports the hypothesis that open-door policy in acute psychiatric units is seen positively by patients and that further research should be carried.
Disclosure of InterestNone Declared
A tale of excess: the curious case of the woman with 1447 emergency visits
- M. Sagué Vilavella, A. Giménez Palomo, A. Àvila-Parcet, T. Fernández Plaza, L. Navarro Cortés, G. Oretega Hernández, M. Pons Cabrera, L. Tardón Senabre, M. Vázquez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S286
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Frequent attenders to emergency services are challenging and costly. We report the case of a woman in her mid-twenties who stands out for a total of 1447 emergency visits.
ObjectivesOur primary objective was to describe the emergency visits of our patient. Secondary objectives were to assess her use of other healthcare services and to calculate her health expenditure.
MethodsThis is a clinical case report. We reviewed the patient’s electronic medical records for sociodemographic and clinical data. We obtained detailed information of psychiatric ED visits (length, most frequent times and days) regarding the second most-visited hospital. We assessed the efficacy of hospitalizations in reducing ED visits with a paired samples t Test, comparing the number of visits 30 days pre- and post-hospitalization. We estimated the health expenditure using the regional public health system prices, including three direct costs: emergency visits, hospitalizations and ambulance transportation. We obtained written informed consent from the patient’s legal guardian.
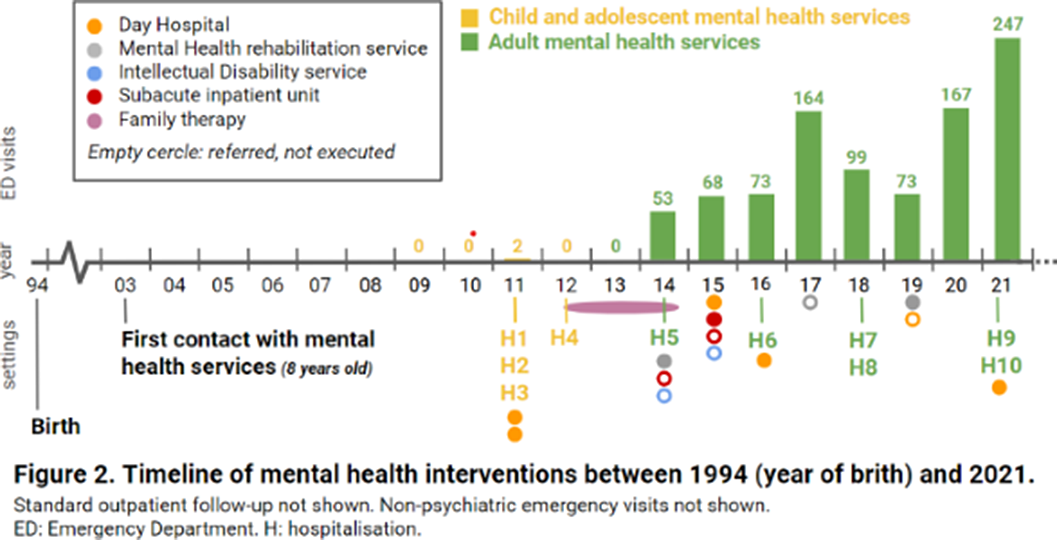
ResultsA 26-year-old woman from Barcelona (Catalonia, Spain), diagnosed with mild intellectual disability, made 1447 emergency visits between 2009 and 2021 (figure 1). 946 visits (65%) took place in psychiatric emergency departments (EDs), whilst 353 (24%) in non-psychiatric EDs and 148 (10%) in urgent primary care. She attended 24 hospitals (ranking number one the closest to the patient’s home, with 387 visits) and seven primary care centers, distributed across 17 cities in Catalonia. Most visits were self-referred, being the main presenting problems anxiety and instrumental suicidal behaviour. Saturday was her favorite day for hospital visits (24,1%), while she seeked care on Tuesdays much less often (4.5%). She made 73.5% of consultations between 1pm and 6pm, with a median length per visit of 2.8 hours (range 0.33-20.9 hours). Regarding other therapeutic approaches, she attended day hospitals, psychiatric rehabilitation programs and family therapy, among others (figure 2), for which she showed low adherence and scarce benefit. She had ten acute hospitalizations, interventions that did not reduce ED visits (t=-0.9835, p=0.36). Health expenditure reached 410.035€.
Image:
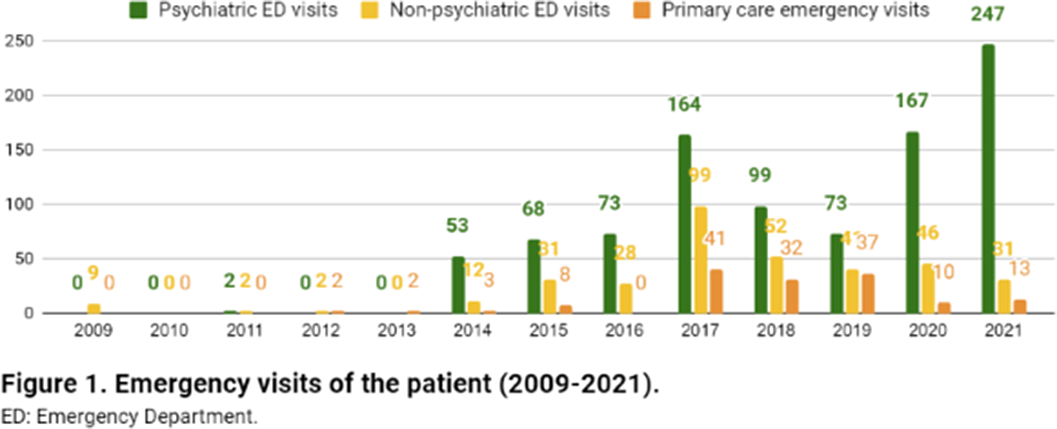
Image 2:
 Conclusions
ConclusionsThe most common definition of frequent attendance is a patient who has five or more visits per year. Many times, but not always, repeat visits are also inappropriate. The case we report is a grotesque example of both frequent and inappropriate attendance, which has been resistant to all kinds of interventions and has quality-of-care, financial and ethical implications. As of today, it is still a pending case. Maybe it is worth considering residential treatment?
Disclosure of InterestNone Declared
Acute psychosis following corticosteroid administration for COVID-19 and Respiratory Syncytial Virus infection: A case study
- E. Miranda Ruiz, E. Marimon Muñoz, J. Ramirez Gonzalez, M. Fariña, R. G. Troyano, M. I. Arroyo Ucar, S. Ferreiro, I. Fernandez Marquez, C. Hidalgo, A. Quispe, L. Delgado
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S790
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Steroids are a necessary treatment for hypoxic respiratory failure; however there are many side effects that should be taken into account. A 44- year-old-woman with asthma and no past psychiatric history was admitted due to COVID-19 pneumonia and Respiratory syncytial virus (RSV) infection, presenting hypoxic respiratory failure. After two days of intravenous methylprednisolone administration, the patient presented acute psychosis and agitation.
It has been previously described that steroid use can cause effects such as mania, anxiety, agitation, delirium and psychosis amongst other. However they are a necessary treatment in respiratory illnesses and are sometimes unavoidable.
ObjectivesThe aim was to examine the appropriate medical response to steroid induced psychosis in patients with acute hypoxic failure.
MethodsA bibliographical review was done in PubMed database searching recent cases of steroid induced psychosis using the words (“Steroid”, “Psychosis” and “COVID-19”).
ResultsAccording to literature, it has been shown that partial or complete reduction of steroid use and/or use of psychotropic has been successfully used to treat steroid induced psychosis. Following the research it was decided to reduce intravenous methylprednisolone dose from 20mg/ 8h to 20mg/12h and start oral haloperidol 5mg/8h the first 24h and reducing the dose progressively as the patient recovered. After the first 24 hours the patient presented adequate response to steroids as well as partial response to antipsychotic treatment; presenting no further agitation, absence of hallucinations and partial persistence of the persecutory delusion. A couple of days later there was complete remission of the psychotic symptoms and the patient was on the way to recovery from COVID-19 and RSV.
ConclusionsThere is evidence that suggests that medications such as steroids used to treat COVID-19 and other respiratory illnesses can lead to psychotic episodes. It is very important to pay attention to possible side effects when treating with steroids and evaluate the patient history as well as suggest having a follow up visit after the hospital discharge.
Disclosure of InterestNone Declared
Acute mutism in a young female. A case report of a 20-year-old female who presents a 3-month mutism
- A. Gonzalez-Mota, A. Gonzalez-Gil, C. Martin-Gomez, J. A. Benito-Sanchez, I. M. Peso-Navarro, L. Fernandez-Alonso
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S177-S178
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A 20-year-old female presents with a progressive 3-month mutism, hyporexia (20kg weight loss), abulia, anhedonia, apathy, social isolation,seeking company of her parents even at night, bradypsychia, sialorrhea, psychomotor slowdown and hypomimia. She is hospitalized in the Psychiatric Brief Hospitalization Unit (PBHU).Her parents relate the beginning of this symptomatology to a breakup and gender violence,which the patient confirms during the interview by eye/cephalic movements and single words jotted down.
ObjectivesThe objective of this study is to describe the evolution of the patient during her hospitalization in the PBHU of Salamanca and to look into the available bibliography about mutism related to stress and sialorrhea.
MethodsWe carried out a follow-up of the hospitalization of the patient and a structured search in PubMed with the keywords “mutism”,“sialorrhea” and “stress” in the last 10 years in English,Spanish and French.
ResultsFew or no articles where found.Therefore, the articles about mutism and stress were analyzed, which focused mostly in selective mutism. Regarding fear,the response to cope with the threat(fight, flight, freeze) is mediated by the autonomic system. The “Polyvagal Theory” speaks about the vagus nerve participating in emotion regulation (social communication and mobilization). Dissociation, in this context,has adaptive and defensive purposes and its threshold can be reduced by repeated stress situations.Long-term alteration of the autonomic nervous system has been described in selective mutism.This malfunction can be related to an elevated production of saliva due to the activation of the parasympathetic in the salivary glands, causing sialorrhea in our patient.
The patient began treatment with sertraline 100mg and risperidone 2mg with the aim of its antidepressive and major tranquilizer effects, she also began individual and family psychotherapy, we assured her sleep and intakes and she began to progressively recover her speech and mobility,identifying a possible trigger for the symptomatology: a physical beating of gender violence after her breakup.
ConclusionsDissociation and “freeze” response can be a maladaptative mechanism to fear.The malfunction of the autonomic nervous system can explain the disconnection,poor gaze,low facial and body expression and inability to speak.
Disclosure of InterestNone Declared
Efficacy of maintenance electroconvulsive therapy in recurrent depression: a case series
- G. Guerra Valera, Ó. Martín Santiago, M. Esperesate Pajares, Q. D. L. de la Viuda, A. A. Gonzaga Ramírez, C. Vallecillo Adame, C. de Andrés Lobo, T. Jiménez Aparicio, N. Navarro Barriga, B. Rodríguez Rodríguez, M. Fernández Lozano, M. J. Mateos Sexmero, A. Aparicio Parras, M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, M. D. L. Á. Guillén Soto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S832
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Maintenance electroconvulsive therapy (mECT) is an option in the treatment of affective disorders which progress is not satisfactory. It is certainly neglected and underused during the clinical practice.
ObjectivesTo evaluate the efficacy of mECT in reducing recurrence and relapse in recurrent depression within a sample of three patients.
MethodsWe followed up these patients among two years since they received the first set of electroconvulsive sessions. We applied the Beck Depression Inventory (BDI) in the succesives consultations for evaluating the progress.
ResultsThe three patients were diagnosed with Recurrent Depressive Disorder (RDD). One of them is a 60 year old man that received initially a cycle of 12 sessions; since then he received 10 maintenance sessions. Other one is a 70 year old woman that received initially a cycle of 10 sessions; since then she received 6 maintenance sessions. The last one is a 55 year old woman that received initially a cycle of 14 sessions; since then she received 20 maintenance sessions.
All of them showed a significant reduction in depressive symptoms evaluated through BDI and clinical examination. In the first case, we found a reduction in the BDI from the first consultation to the last that goes from 60 to 12 points; in the second case, from 58 to 8 points; and in the last case, from 55 to 10 points. The main sections that improved were emotional, physical and delusional.
As side-effects of the treatment, we found anterograde amnesia, lack of concentration and loss of focus at all of them.
ConclusionsWe find mECT as a very useful treatment for resistant cases of affective disorders like RDD.
It should be considered as a real therapeutic option when the first option drugs have been proved without success.
Disclosure of InterestNone Declared
Gut permeability and low-grade inflammation in bipolar disorder
- M. Couce, G. Paniagua, L. González-Blanco, A. García-Fernández, C. Martínez-Cao, P. Sáiz, J. Bobes, M. P. García-Portilla
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S385-S386
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Systemic inflammation has been increasingly related to bipolar disorder -BD- (Tanaka et al. Neurosci Res 2017;115 59-63). Intestinal bacterial translocation has been postulated as one of the causes of this inflammation (Nguyen et al. J Psychiatr Res 2018;99 50-61). A possible pathway is through the lipopolysaccharide, which is presented to CD14 through lipopolysaccharide binding protein (LBP) leading to a release of systemic inflammatory markers like C-reactive protein (CPR) (Funda et al. Infect Immun 2001;69 3772-81).
Objectives1) Describe gut permeability in patients with BD through the determination of intestinal inflammatory markers (LBP, sCD14) in plasma; 2) Analyze variables associated with intestinal inflammation.
MethodsCross-sectional study of 38 patients with BD [mean age=45.50 (SD=10.93; range 23-68); males=15 (39.5%)], recruited from mental health outpatient clinics in Oviedo (Spain).
Assessment: Pro-inflammation biomarkers [CRP (mg/dL), Erythrocyte Sedimentation Rate (ESR) (mm/h), Neutrophil/Lymphocyte, Monocyte/Lymphocyte, Platelet/Lymphocyte and Systemic Immune Inflammation Indexes]. Indirect markers of intestinal bacterial translocation [LBP, soluble CD14 (sCD14)]. Dichotomous variables were created for LBP, considering LBP ≥15 μg/dL as increased gut permeability; and for CPR, considering CRP≥0.3 as systemic inflammation. Metabolic syndrome [ATPIII criteria: glucose, HDL, triglycerides (mg/dl), arterial pressure (mmHg), abdominal circumference (cm)], body mass index (BMI) (kg/m2), smoking, cannabis or alcohol use.
Statistical analyses: t-Student test, multiple linear regression analyses.
ResultsAverage LBP was 14.60 μg/dL (SD=6.4) and 15 patients (39.5%) had increased gut permeability. Moreover, average CPR was 0.40 mg/dL (SD=0.58) and 16 patients (47.1%) showed systemic inflammation. There were no patients with increased levels of sCD14.
Associations were found between LBP and CPR (r=0.357; p=0.032), cannabis use in the last month (t=-2.293; p=0.029), BMI (r=0.433; p=0.008) and abdominal obesity (t=3.006; p=0.005); but no with age or sex.
Subsequently, a multiple linear regression model for LBP was calculated with variables previously mentioned, and age (based on expert criteria). The overall regression was statistically significant (R2=0.49, F=9.273, p<0.001). It was found that CPR, abdominal obesity, and cannabis use in the last month significantly predicted LBP levels (table 1).
Table 1. Multiple linear regression analyses to LBP B SE β t p CPR 4.842 1.529 0.439 3.167 0.004 Abdominal obesity 4.810 1.849 0.362 2.601 0.014 Cannabis use -5.048 2.273 -0.296 -2.221 0.034 ConclusionsMore than one third of patients with BD had increased gut permeability. Almost 50% had systemic inflammation. Intestinal permeability was directly related to abdominal obesity and systemic inflammation, but inversely related to cannabis use.
Disclosure of InterestNone Declared
UNTIL IT BURSTS OR ALL OF US BURST. A SCHIZOTYPICAL CASE.
- B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, A. Aparicio Parras, M. D. L. Á. Guillén Soto, T. Jiménez Aparicio, M. D. C. Vallecillo Adame, C. de Andrés Lobo, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Queipo de Llano de la Viuda, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S967
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizotypal disorder is conceptualized as a stable personality pathology (Cluster A) and as a latent manifestation of schizophrenia. It can be understood as an attenuated form of psychosis or high-risk mental state, which may precede the onset of schizophrenia or represent a more stable form of psychopathology that doesn’t necessarily progress to psychosis.
ObjectivesTo exemplify the continuum of psychosis
MethodsReview of scientific literature based on a relevant clinical case.
Results39-year-old male living with his parents. He started studying philosophy. He is a regular cannabis user and has an aunt with schizophrenia. He’s admitted to psychiatry for behavioral disturbance in public. He refers to having been hearing a beeping noise in his street for months, what he interprets as a possible way of being watched due to his past ideology. Without specifying who and why, he sometimes shouts “until it bursts” to stop the noise and he thinks that his neighbours alerted the police about his behavior. During the interview he alludes to Milgram’s experiment, saying that throughout history there have been crimes against humanity and those who pointed them out were labeled “crazy”. His father refers that he has always been “strange” and with certain extravagant revolutionary ideas and thoughts. He doesn’t maintain social relationships and dedicates himself to reading and writing.
ConclusionsIt’s important to understand psychosis as a continuum to advance the understanding of etiology, pathophysiology and resilience of psychotic disorders and to develop strategies for prevention and early intervention
Disclosure of InterestNone Declared
Delirious episode secondary to rotigotine: the psychotic patch
- M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, P. Pando Fernández, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, T. Jiménez Aparicio, M. D. C. Valdecillo Adame, C. de Andrés Lobo, G. Guerra Valera, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramirez, M. D. L. Á. Guillén Soto, A. Aparicio Parras, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S626
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a fine line separating psychiatry and neurology. Most movement disorders can have psychiatric symptoms, not only those caused by the disease itself, but also those induced by the drugs used to treat them.
ObjectivesPresentation of a clinical case about a patient diagnosed with Parkinson’s disease presenting a several-month-long delirious episode due to dopaminergic drugs.
MethodsLiterature review on drug-induced psychosis episodes in Parkinson’s disease.
ResultsA 57-year-old patient with diagnosis of Parkinson’s disease for six years, who went to the emergency room accompanied by his wife due to delirious ideation. He was being treated with levodopa, carbidopa and rasagiline for years, and rotigotine patches whose dosage was being increased over the last few months.
His wife reported celotypical clinical manifestations and multiple interpretations of different circumstances occurring around her. He chased her on the street, had downloaded an app to look for a second cell phone because he believed she was cheating on him, and was obsessed with sex. He had no psychiatric background. It was decided to prescribe quetiapine.
The following day, he returned because he refused to take the medication since he thought he was going to be put to sleep or poisoned. It was decided to admit him to Psychiatry.
During the stay, rasagiline and rotigotine were suspended. Olanzapine and clozapine were introduced, with behavioral improvement and distancing from the psychotic symptoms which motivated the admission. The patient was also motorically stable. Although levodopa is best known for causing psychotic episodes, the symptons were attributed to rotigotine patches for temporally overlapping the dose increase.
ConclusionsPsychiatric symptoms are the third most frequent group of complications in Parkinson’s disease after gastrointestinal complications and abnormal movements. All medication used to control motor disorders can lead to psychosis, not only dopaminergics, but also selegiline, amantadine and anticholinergics.
Excessive stimulation of mesocortical and mesolimbic dopaminergic pathways can lead to psychosis, which is the most common psychiatric problem related to dopaminergic treatment.
In the face of a psychotic episode, antiparkinsonian drugs which are not strictly necessary for motor control should be withdrawn. If this is not sufficient, levodopa dose should be reduced, considering the side effects that may occur. When the adjustment of antiparkinsonian treatment is not effective, neuroleptics, especially quetiapine or clozapine, should be administered. In a recent study, pimavanserin, a serotonin 5-HT2 antagonist, was associated with approximately 35% lower mortality than atypical antipsychotic use during the first 180 days of treatment in community-dwelling patients.
Medication should always be tailor-made to suit each patient and we usually have to resort to lowering or withdrawing the dopaminergic medication.
Disclosure of InterestNone Declared
Brief intervervention for a metabolic syndrome in psychiatric outpatients with severe/persistent mental illness: A prospective study
- M. Escarti, C. Alonso, L. Fernandez, O. Ribera, A. Beato, R. Cozar, G. Selva
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S904
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Metabolic syndrome and other cardiovascular risk factors are highly prevalent in people with mental severe illness (Sun & Jang, 2020).Metabolic disorders in people with schizophrenia increase their risk of developing cardiovascular disease, consequently reducing their life expectancy by approximately 10 to 25 years (Heald et al., 2017)In part these cardio-metabolic risk factors are attributable to unhealthy lifestyle, including poor diet and sedentary behaviour.Lifestyle interventions (diet, increased physical activity) are the first-line treatments to decrease that risk.
ObjectivesOur objective is to carry out a prospective study on the application of a program of healthy habits in outpatients unit
MethodsPatients with mental severe illness were recruited at a mental health center in the Hospital Clinic of Valencia. Inclusion criteria: age from 18 to 65 years and diagnosis of severe/persistent mental illness Exclusion criteria: acute illness, were not understanding Spanish, not be able to read and understand questionnaries. We included following data: sociodemographic data and aspects of the health behaviors, anthropometric measurements and analytical with hemogram and biochemistry pre and post-intervention. All subjects gave informed consent for participation in the study.
ResultsWe included 12 patients, but only 9 completed the full program. Average baseline data suggests that participants were at increased health risk when entering the program.At the end of the program, differences were observed: a reduction in glucose profile, a reduction of an average of 3.33 kg from the initial weight and a reduction of 10 points in blood pressure.
ConclusionsThis real world pilot trial evaluate of a health promotion intervention targeting physical activity and healthy eating in mental health care using a specific programme.
Disclosure of InterestNone Declared
I don’t know where I’m going or where I come from. Self-disorders in schizophrenia.
- M. D. C. Vallecillo Adame, L. Rodríguez Andrés, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramirez, M. Fernández Lozano, M. J. Mateos Sexmero, N. Navarro Barriga, B. Rodríguez Rodríguez, M. P. Pando Fernández, M. Calvo Valcárcel, P. Martínez Gimeno, M. A. Andreo Vidal, I. D. L. M. Santos Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1069-S1070
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In the early stages of schizophrenia the person experiences feelings of strangeness about themselves, difficulty in making sense of things and difficulty in interacting with their environment. Based on this, self-disorder assessment instruments have been developed and empirical studies have been conducted to assess people at risk of developing a schizophrenia spectrum disorder. These studies show that self-disorders are found in pre-psychotic stages and that their manifestation can predict the transition to schizophrenia spectrum disorders.
ObjectivesWe present the case of a patient with multiple diagnoses and mainly dissociative symptoms who, after years of evolution, was diagnosed with schizophrenia.
MethodsBibliographic review including the latest articles in Pubmed about self-disorders and schizophrenia.
ResultsWe present the clinical case of a 51-year-old woman with a long history of follow-up in mental health consultations and with multiple hospital admissions to the psychiatric unit, with several diagnoses including: dissociative disorder, histrionic personality disorder, adaptive disorder unspecified psychotic disorder and, finally, schizophrenia. The patient during the first hospital admissions showed a clinical picture of intense anxiety, disorientation and claiming to be a different person. The patient related these episodes to stressors she had experienced, and they improved markedly after a short period of hospital admission. Later, psychotic symptoms appeared in the form of auditory and visual hallucinations and delusional ideation, mainly of harm, so that after several years of follow-up and study in mental health consultations and in the psychiatric day hospital, she was diagnosed with schizophrenia and treatment with antipsychotics was introduced, with a marked clinical improvement being observed.
ConclusionsIt is important to take into account this type of symptoms (self-disorders), as they allow the identification of individuals in the early stages of the disorder and create the opportunity for early therapeutic interventions.
Disclosure of InterestNone Declared
Relationship between CAINS negative symptoms and cognition, psychosocial functioning and quality of life in patients with a first psychotic episode of schizophrenia
- R. Rodriguez-Jimenez, L. García-Fernández, V. Romero-Ferreiro, M. Valtueña García, A. I. Aparicio, J. M. Espejo-Saavedra, L. Sánchez-Pastor, A. Nuñez-Doyle, M. Dompablo, O. Jiménez-Rodríguez, D. Rentero, P. Fernández-Sotos, I. Martínez-Gras, J. L. Santos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S641-S642
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Negative symptoms has been classically associated with cognition, psychosocial functioning and quality of life in patients with schizophrenia. But negative symptoms are not a unitary construct, encompassing two different factors: diminished expression, and motivation and pleasure. Few works have studied the relationship between these two different negative symptoms factors and cognition (neuro and social cognition), psychosocial functioning and quality of life, jointly, in patients with a first psychotic episode of schizophrenia.
ObjectivesThe objective of the present work was to study, in a sample of patients with a first psychotic episode of schizophrenia, the relationship between the negative symptoms (diminished expression and motivation and pleasure) and neurocognition, social cognition, functioning and quality of life.
MethodsThe study was carried out with 82 outpatients with a first psychotic episode of schizophrenia from two Spanish hospitals (“12 de Octubre” University Hospital, Madrid and “Virgen de la Luz” Hospital, Cuenca). The patients were assessed with the Clinical Assessment Interview for Negative Symptoms (CAINS) for evaluating diminished expression (EXP) and motivation and pleasure (MAP) symptoms, the MATRICS Consensus Cognitive Battery (MCCB) for evaluating neurocognition and social cognition, the Social and Occupational Functioning Assessment Scale (SOFAS), and the Quality of Life Scale (QLS).
ResultsA negative correlation was found between neurocognition and the two negative symptoms subscales: CAINS-EXP (r=-0.458, p<0.001) and CAINS-MAP (r=-0.374, p<0.001); but with social cognition only CAINS-EXP was correlated (r=-0.236, p=0.033). Also, it was found a high negative correlation between SOFAS scores and CAINS-MAP (r=-0.717, p<0.001); and a medium negative correlation with CAINS-EXP (r=-0.394, p<0.001). Finally, QLS score was high correlated with both CAINS subscales: CAINS-EXP (r=-0.681, p<0.001) and CAINS-MAP (r=-0.770, p<0.001).
ConclusionsThis study found a relationship between negative symptoms and neurocognition, social cognition, functioning and quality of life in a sample of patients with a first psychotic episode of schizophrenia. But the two different negative symptom factors, diminished expression, and motivation and pleasure, are associated differently with psychosocial functioning, but especially with social cognition where the relationship was only found with diminished expression symptoms.
Disclosure of InterestNone Declared
Late diagnosis of attention deficit hyperactivity disorder and cocaine abuse
- C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. Fernández Lozano, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Calvo Valcárcel, M. Andreo Vidal, M. P. Pando Fernández, P. Martínez Gimeno, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S335-S336
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Adult ADHD diagnosis sometimes represents a challenge for the clinician, due to the comorbid psychiatric diseases that are often associated and which complicate de recognition of the primary symptoms of ADHD. The prevalence of ADHD in adult populations is 2’5% and it is a relevant cause of functional impairment.
ObjectivesPresentation of a clinical case of a male cocaine user diagnosed with adult ADHD.
MethodsLiterature review on adult ADHD and comorbid substance abuse.
ResultsA 43-year-old male who consulted in the Emergency Department due to auditory hallucinosis in the context of an increase in his daily cocaine use. There were not delusional symptoms associated and judgment of reality was preserved. Treatment with olanzapine was started and the patient was referred for consultation. In psychiatry consultations, he did not refer sensory-perceptual alterations anymore, nor appeared any signals to suspect so, and he was willing to abandon cocaine use after a few appointments. He expressed some work concerns, highlighting that in recent months, in the context of a greater workload, he had been given several traffic tickets for “distractions.” His wife explained that he had always been a inattentive person (he forgets important dates or appointments) and impulsive, sometimes interrupting conversations. In the Barkley Adult ADHD Rating Scale he scored 32 points.
He was diagnosed with adult ADHD and treatment with extended-release methylphenidate was started with good tolerance and evolution, with improvement in adaptation to his job and social environment. Since then, the patient has moderately reduced the consumption of drugs, although he continues to use cocaine very sporadically.
ConclusionsEarly detection of ADHD and its comorbidities has the potential to change the course of the disorder and the morbidity that will occur later in adults. Comorbidity in adult ADHD is rather the norm than the exception, and it renders diagnosis more difficult. The most frequent comorbidities are usually mood disorders, substance use disorders, and personality disorders. Treatment of adult ADHD consists mainly of pharmacotherapy supported by behavioral interventions. When ADHD coexists with another disorder, the one that most compromises functionality will be treated first and they can be treated simultaneously. The individual characteristics of each patient must be taken into account to choose the optimal treatment.
Disclosure of InterestNone Declared






